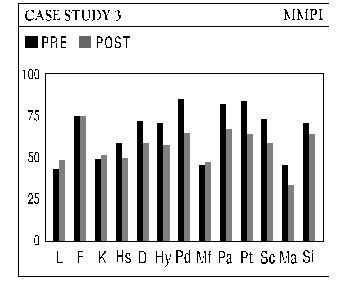|
ALPHA-THETA NEUROTHERAPY AS A MULTI-LEVEL MATRIX OF INTERVENTION
Nancy E. White, Ph.D. and Karinn Martin, M.S.W.
The Enhancement Institute Houston, Texas
ABSTRACT
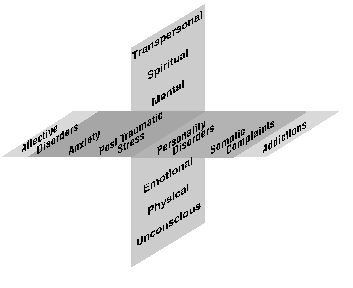
Alpha-Theta Neurotherapy, has been found in clinical practice, as in the original work of Elmer and Alyce Green and further developed by Eugene Peniston and described in his original research, to reduce or eliminate alcoholic craving while simultaneously addressing mental, emotional, physical and, at times, spiritual dimensions of alcoholism and surrounding issues. The Peniston protocol of Alpha-Theta Neurotherapy is treated as a multilevel matrix by addressing multiple diagnoses of affective disorders, anxiety, post traumatic stress disorders, personality disorders and some somatic complaints while simultaneously addressing the chemistry of addiction.
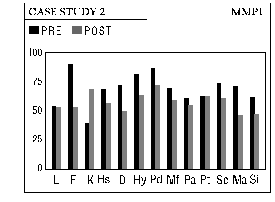
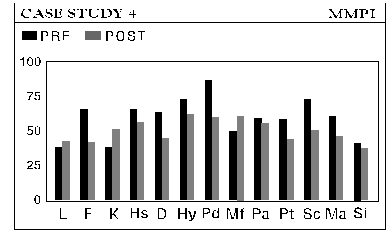
The methodology of the Peniston protocol involves pre and post treatment testing using the Minnesota Multiphasic Personality Inventory (MMPI-2) and the Millon Clinical Multiaxial Inventory II (MCMI-II), thermofeedback training to attune autogenic responses, the development and use of imagery with respect to both the process and the desired outcome, and a prescribed regimen of EEG Neurofeedback using specific neurological training sites. The patient is encouraged to practice a post treatment regimen of regular meditation with imagery of desired outcome along with periodic "booster" sessions if indicated. One year of periodic follow-up is advocated to monitor the progress of the patient.
The previous high recidivism rates of alcoholics with multiple diagnoses (comorbidity) may stem from failure to adequately address underlying psychological disorders in the treatment process. The Peniston protocol facilitates the release of deep unconscious material while the patient is in a predominant theta brainwave state. While the etiology of comorbidity is unknown, it could be related to neurochemical imbalances that may either precede, succeed or coincide with alcoholism. One of the reasons for the Peniston protocol's success may be related to this possibility, since both alcoholism and emotional conditions may be considered in terms of neurochemical transactions. Use of prescription drugs to alleviate symptoms, while necessary in certain cases, may be ineffective and contraindicated in other cases and could be double-edged: it may lead back to the dependence on the drug of choice and/or create conflict with programs demanding abstinence.
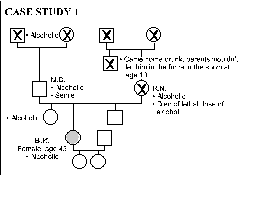
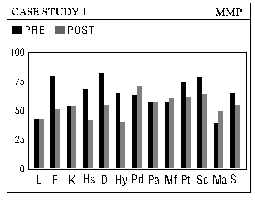
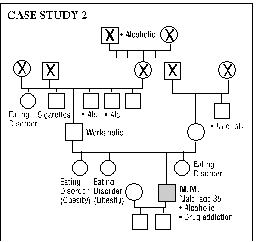
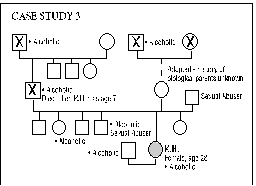
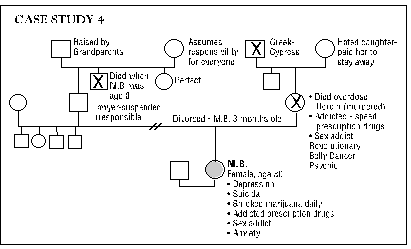
Four case studies from the files of The Neurotherapy Center are presented as examples of the presenting problems and their degree of resolution. The authors then present the theories of Colin Wilson (Chronic Trauma), Stanislav Grof (COEX Systems), Bruce Perry (effects of prolonged "alarm reactions"), Rossi and Cheek (state-dependent learning and memory) expanded by Cowan, and Alyce and Elmer Green (Beyond Biofeedback), among others, to help rationalize the exceptional effectiveness of the Peniston protocol in treating multiple disorders with accompanying addiction. A final discussion expands these ideas and brings in the experiences of actual patients, noting the "letting go" that accompanies access to slow brainwave states, ultimately allowing entry into a nonlocal reality (outside of linear space and time). Within this nonlocal reality, one's awareness of self becomes distinct from the conscious ego and one may experience "inner guidance" by means of which, frequently in a dream or "vision," one may release unconscious material, heal psychic wounds and subsequently experience a change in one's phenomenal world. The authors see the ability to promote these outcomes, and the power of the protocol, in effect, as resting in training the patient to enter and hold a deep slow brainwave state simultaneously with intention of a desired outcome. Implied is the possibility that cogent intent, held in the slow brainwave state, can produce shifts in neurochemistry.
INTRODUCTION AND BACKGROUND
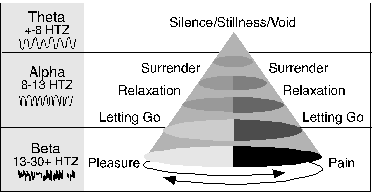
In March of 1989, when Eugene Peniston's and Paul Kulkosky's research was published in Medical Psychotherapy, it may have heralded a major shift in the future course of therapy for addictions. Their research amplified the prior work of Elmer and Alyce Green, Dale Walters, Margaret Ayers, Barbara Brown, Joe Kamiya, Les Fehmi, Tom Budzynski and others over the past twenty plus years. The Peniston Protocol created a multilevel matrix approach which could simultaneously treat the multiple diagnoses of affective disorders, anxiety, post traumatic stress disorders, personality disorders, some somatic complaints and addiction (Peniston, 1989, 1990, 1991) comprising the horizontal axis with the unconscious, the physical, emotional, mental, spiritual and transpersonal forming the vertical axis. Computerized EEG feedback, a therapeutic relationship and the imagery of desired outcome, interfaced technology with compassionate personal contact. This protocol worked concurrently on overlapping addictions and the underlying psychological state.
Figure 1. The Peniston Protocol creates a multilevel matrix of intervention with its horizontal axis of diagnoses & presenting problems & its vertical axis of levels of the Self & Self connected to All That Is.
The April, 1991 issue of Men's Health magazine commented on a study reported in the Journal of the American Medical Association
"Why do many alcohol or drug addicts repeatedly sober up, only to relapse? They may be suffering from underlying preexisting mental illness, including manic-depressive and anxiety disorders, depression and schizophrenia.
"A recent study conducted by the Federal Alcohol, Drug Abuse and Mental Health Administration and published in the Journal of the American Medical Association (JAMA) points up the futility of repeatedly detoxifying addicts without addressing their mental problems. Researchers also find that psychological treatment is useless while a mentally ill person is abusing drugs or alcohol. The answer appears to be tackling the symptom and the underlying cause simultaneously."
As many as 30% of all individuals treated for chemical dependency and 50% of all individuals treated for psychiatric/psychological disturbances may be suffering from both a chemical problem and mental illness (Continuum, 1993). JAMA states that among those with an alcohol disorder the lifetime prevalence of at least one other mental disorder was 70%. The highest comorbidity rates are for affective, anxiety, and antisocial personality disorders (Regier, 1990).
Dual diagnosis patients are difficult to treat and have high recidivism rates according to an article by Wolpe, Gorton, Serota, and Sanford in Hospital and Community Psychiatry, January, 1993. Levy and Mann reported in the Journal of Substance Abuse Treatment in 1988: "Dually diagnosed patients have problems beyond alcoholism that complicate recidivism; problems in regulating thought, affect, and behavior; poor self-esteem; and low frustration tolerance among others" (Continuum, 1993).
From a scientific perspective, the etiologic mechanisms underlying these high rates of comorbidity remain undiscovered. Common neurotransmitter systems have been identified for some mental and addictive disorders. For example, dopamine system dysfunction has long been considered a factor in certain forms of mental illness and dopamine-mediated psychological reward and reinforcement functions have been demonstrated more recently to be related to substance abuse (Ritz, 1987). The system for producing and distributing serotonin also has been critical to the understanding and treatment of affective disorders (Goodwin, 1973), and decreased serotonin metabolite levels have been found in the more aggressive and impulsive population of young male alcoholics (Ballenger, 1979). Evidence also suggests that certain mental disorders such as affective and anxiety disorders may precede the development of substance abuse problems, although there is increasing argument that certain mental disorders are actually the result rather than the cause of substance abuse disorders (Schuckit, 1988). It is difficult to ascertain which came first, the addiction or the mental illness, or were they born hand in hand through some imbalance in the neurochemistry (Blum, 1991) and/or core trauma?
It is not uncommon for addicts to present depressive symptoms prior to addiction and, if not that, they may have feelings of worthlessness and guilt about what they have created out of their chronic addiction. The recovering addict is often anxious. Suicidal ideation, especially in the addict detoxing from cocaine, is also encountered. Recovering individuals often report that they feel worse than they did when they were using. Their behavior is still addictive with the major change being that they are no longer using their drug of choice. Often they exhibit personality disorders.
One way of treating this problem of dual diagnosis, or perhaps multiple diagnosis, has been to give the patient drugs. The presence of medication can interfere with the treatment of addiction. Addicts may have come in with the desire to get off drugs and not to use anymore, but use the prescribed medication as an excuse to sabotage their treatment. Perhaps pleased to not have to go chemical free, the addict could assume that since the doctor prescribed medication that the doctor must agree that he or she can't live chemically free in order to function. Any regularly prescribed medication could lead to this thinking process. So, addicts may rationalize that, since they can't live chemically free, they may as well take their drug of choice rather than the prescribed chemical (Reilly, 1989; Sweben, 1993).
There are considerations concerning medication in another direction as well. Compliance with an aftercare program is strongly associated with improved outcomes, lowering the recidivism rate. A strong support system is an important factor (in recovery), yet many twelve step groups such as A.A. (Alcoholics Anonymous), C.A. (Cocaine Anonymous) and N.A. (Narcotics Anonymous) view the use of even essential psychotropic medications as "using" or not remaining substance-free. This leads to conflict with sponsor and/or group support and possibly damaging compliance with the prescribed drug regimen. Many times these patients simply return to the former situation, which often leads to a return of their addiction and mental/emotional symptoms. (Continuum, 1993; Erickson, 1991).
We are not speaking against medication; sometimes it proves to be the best way of handling the multiple diagnosis problem. If there is an effective way to promote what appears to be more permanent healing and recovery without medication, however, we would prefer it.
TREATMENT METHODOLOGY
At The Neurotherapy Center we have found that the Peniston Protocol of Alpha/Theta neurofeedback has allowed us to affect addictive craving directly and to simultaneously address physical, emotional, mental and, sometimes, spiritual levels of the disease. Since emotional problems, as well as addictive craving, may ultimately be explainable in terms of neurochemical transactions, by extrapolation we can speculate that the protocol works to alter the nature of some of these transactions in a lasting way; but this has yet to be proven. Even though the exact mechanisms by which this breakthrough protocol works are not yet known, the method is producing a high level of positive clinical results. For example, a recent survey of several of the leading practioners using Alpha-Theta Neurotherapy estimates that the success rate of outpatient treatment is in the range of 60 to 70%, while the inpatient success rate is in the range of 70 to 80% (Walters,1994). We wish to present a method of treating with this multileveled matrix of healing and to offer actual case studies as examples of achievable outcomes. Later in the Chapter we offer some ideas, based on some leading theories, as to what may make the Peniston protocol so effective.
Our treatment incorporates the protocol developed by Peniston (1989, 1990, 1991), with allowances made for our outpatient clinical setting, and is developed in the following paragraphs. The outpatient model we have developed leaves the Peniston protocol virtually intact. Imagery, while following the guidelines of the protocol, may be directed more to a patient's specific needs and presenting problems. A minimum of four treatments per week is indicated, scheduled to recognize to the extent possible the demands of the patient's outside life. Severe cases may receive two treatments per day, with a minimum three-hour interim between treatments, up to four days a week. The accelerated pace may continue just for the first several weeks of treatment or may last the entire time. Adjunctive treatment may be called for in certain cases, such as individual psychotherapy and/or CES treatments. When we treat an addict from another city we help them find living arrangements conducive to sobriety - often a halfway house that understands our program - and assist them in joining a support group, either one of our own or another. We also conduct random drug and alcohol testing on addicts during the course of treatment.
Intake and Assessment
The initial phase of assessment utilizes the Peniston procedures which involve:
1. Pre-treatment psychological testing: Patients complete The Minnesota Multiphasic Personality Inventory-2 (MMPI-2) and The Millon Clinical Multiaxial Inventory II (Millon II) prior to beginning the treatment.
2. Medical history
3. Addiction history
4. Neurological conditions including any head trauma history
5. Personal history
(with emphasis on any mental, emotional or physical trauma, particularly in childhood)
6. Needs and goals of the patient assessed
7. Explanation of the program
8. Patient commitment to the program
Pre-Treatment
Patients complete the MMPI-2 and the Millon II and fill out a personal, medical and addiction history, a neurological checklist and completes a quantative EEG prior to beginning treatment. We then meet with the patient to review the outcome of these assessments. At this time an overview of the EEG brainwave training is explained. The needs and goals of the patient are assessed and any mental, emotional or physical traumas of childhood are discussed.
Thermofeedback Training
The Peniston protocol begins with four to six thirty-minute sessions of thermal biofeedback-assisted autogenic training. The subject is instructed to sit in an Alpha chair (manufactured by Sensory Environment Engineers) and to relax with eyes closed. These chairs are used to accelerate/heighten the patient's auditory stimuli and create a feeling of environmental security. The Alpha chair is a cushioned egg-shaped chair with strategically placed speakers wrapping their sounds around the occupant. A temperature sensor is attached to the middle finger of the subject's dominant hand, collecting data received by a J&J I-330 instrument. Autogenic phrases are presented to the patient by way of an audio tape. Individuals who are auditorily non-responsive are assisted in creating effective visualizations for themselves instead. The patient is taught deep rhythmic breathing techniques to induce relaxation of the body and to quiet the mind. A training criterion of warming the hands to between 94 and 96 degrees Fahrenheit is established.
Imagery Development
Following the thermal training but prior to the brainwave training, one session is devoted to the clarification of the patient's goals and imagery is constructed to represent the patient's desired outcome. An alcohol rejection scene is developed relevant to the patient's previous drinking behavior (Peniston, 1989; Fahrion, 1992). The patient is shown a picture of delta, theta, alpha, and beta brainwaves with an explanation of the state of consciousness that predominance of each of these brainwaves represents. Next he or she is instructed to visualize initially increasing the amplitude of their alpha brainwaves and is told that at some point during the feedback sessions that the alpha amplitude will usually begin to recede and the theta amplitude will rise. The exception to this instruction would be the patient who initially has very high alpha amplitude, in which case the alpha audio feedback will be turned off and they will be instructed to visualize increasing the amplitude of the theta brainwaves from the beginning of the feedback sessions. The next task includes the visualization of one's hypothalamus gland in the center of the brain and requesting that it optimally balance the production of neurotransmitters. The patient is then assisted to create an image of his/her ideal self as he/she wants to be, handling in a positive way the important personality and social issues in his or her life. Next the patient is told, "Let yourself sink down to a state just before sleep without going to sleep." The final step is a directive to the subconscious stating, "Please bring to me anything out of my past that I may need to see or experience for my healing," and then, lastly, giving the simple command of "DO IT!"
Neurofeedback Therapy
The patient is then given 24 to 26 sessions of alpha-theta EEG feedback, a total of 30 sessions overall although additional sessions may be indicated for some individuals. The most common schedule is four sessions of brainwave training per week with a duration of 45 minutes to an hour each which incorporates 30 minutes of active feedback. The patient is instructed to differentiate the alpha and the theta audio feedback tones. The patient sits in a semi-darkened room, in a comfortable reclined chair with the eyes closed and is generally left alone during the active feedback period. The clinician remains nearby in order to make any threshold changes (explained further below) that might become necessary, or to handle any problems. The process of the patient is not interrupted during the feedback session but with a few patients who were inclined to go to sleep, the clinician was available to lightly tap them on the arm to bring them back from sleep. The clinician might suggest that the patient incorporate, "Tell your unconscious mind to keep you awake during the session."
While there are a number of good computerized EEG systems on the market, we have been using the CapScan Prism Five (CapScan Corporation) to monitor the EEG and provide harmonic auditory feedback. The feedback is presented from the left occiput (Green, 1977, Peniston, 1989). Three active, user defined, bandpass filters are set at theta (4-8 Hz), alpha (8-13 Hz) and beta (13-26 Hz). Auditory feedback is provided for alpha and theta independently when brainwave frequency exceeds thresholds. A concurrent bar graph is shown on the screen during the patient's alpha-theta training experience. At the end of each session, a statistical analysis and graph is produced of the mean amplitudes of theta, alpha and beta and is reviewed with the patient.
Earlobes, forehead and scalp are cleansed with alcohol and rubbed with Omni Prep and White Signa Cream used to reduce electrode resistance prior to applying the monopolar electrodes. Electrodes are then placed on FP1, FP2, O1, O2 (International 10-20 placement, Jasper, 1958) and a ground electrode placed midway between FP1 and FP2 and reference electrodes placed on both earlobes. The electrodes are held in place by velcro and a headband.
Electrode impedance is checked before recording begins and electrodes are reapplied accordingly for an impedance of less than 5,000 ohms. Thresholds for alpha and theta are set in order to provide feedback, triggered if the occipital (O1) alpha or theta go above these preset thresholds. Thresholds are adjusted appropriately throughout treatment maintaining approximately 70% feedback. The initial increase of alpha amplitude seems to enable the subject to release physical and mental tension, whereby a deeper, or theta, state of mind surfaces. As the alpha state deepens, the individual lets go of the waking ego state, thus evoking the "window" to the subconscious as theta becomes dominant.
The desired ratio of theta amplitude over alpha amplitude is 2:1. While most alcoholics have low amplitude alpha, we have found that some exhibit high amplitude alpha initially. In these cases, since the original software had no capacity to set an inhibit or to support ratio training, the alpha feedback was eliminated or set above the patient's average amplitude in order to avoid reinforcing excessive alpha production. When the patient begins to produce a predominance of theta brainwaves, a "crossover" occurs (theta at a higher amplitude than alpha). Once crossovers begin to occur regularly, perceptual and behavioral shifts become evident, cravings diminish or disappear and abreactions related to repressed subconscious material emerge. These abreactions seem to emerge naturally in approximately 40 to 60% of the patients with no coaxing from the clinician except the previously stated suggestion, "Please bring me anything of my past that I may need to see or experience for my healing."
At the beginning of the session, as the electrodes are being placed on the patient's head, any relevant issues are processed that may have come up since the last brainwave training session. At the end of the session, the clinician is available to process any abreactions or experiences that the patient had during the session. The clinician listens, not interpreting but allowing the patient to find their own insights. (As a general rule, the patient is not interrupted during the feedback.) The patient is then asked to fill out a post treatment session form which inquires as to their experience during the session. This writing seems to assist the patient in returning to normal waking consciousness (beta dominant) and helps them to integrate whatever experience they had during the session. It also provides a record for them and us to follow their progress.
|