Electrode Placement: One triode surface electrode is placed vertically under the chin. The two active electrodes are aligned centrally, spaced evenly between the inferior tip of the mandible and the thyroid cartilage (figure 5). Palpation is required for accurate placement.
Figure 5
Modified Valsalva / Effortful Swallows
A common diagnostic finding in the dysphagic population is decreased or weakened contraction of the pharyngeal constrictors responsible for propulsion of the bolus through the pharynx. Weakness of these muscles results in post-swallow pharyngeal residual of the bolus, placing the patient at risk for post swallow aspiration. A modified valsalva swallow, or hard swallow can be used as a compensatory strategy to aid pharyngeal clearing during a meal and also as an indirect exercise for increasing pharyngeal constriction. The superior, middle and inferior constrictors are internal pharyngeal muscles that are not easily accessible by surface electrode. Direct EMG measurement of these muscles is not feasible. Although further investigation is required to specifically document the correlation, clinical practice demonstrates a functional relationship between increased pharyngeal constriction and contraction of the submandibular musculature. Thus, in focusing treatment on increased pharyngeal contraction, the electrodes are placed to target the suprahyoid musculature. This muscle group specifically includes the anterior belly of digastric muscle, the stylohyoid muscle, and the mylohyoid muscle. Collectively, these muscles are responsible primarily for elevation of the larynx and tongue and anterior displacement of the cricoid, hyoid, larynx, trachea and tongue. The stylohyoid adds a component of posterior displacement of the above structures with obliteration of the oropharynx.
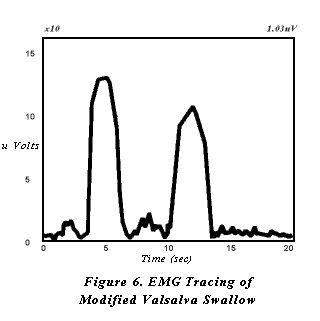
The patient should initially be educated clearly as to the nature of swallowing impairment and the goals of intervention. The therapist demonstrates the technique on his or herself with biofeedback monitoring in place. After electrodes are placed on the patient, he or she is then asked to attempt the strategy by swallowing hard and tightening the muscles in the neck and shoulders during the swallow. The patient is cued to produce high EMG peaks of short duration on the video monitor (figure 6). The treatment objective is production of increasingly higher readings. A quota for expected increase is set for each treatment session. Changes in readings are graphed to document progress.
Mendelsohn Maneuver
The superior point of entry into the esophagus is marked by the cricopharyngeal sphincter muscle (upper esophageal sphincter). In normal swallowing, this sphincter muscle remains tightly closed until the occurrence of the swallow. Vagus nerve innervation and laryngeal elevation jointly contribute to a momentary opening of the cricopharyngeal sphincter, allowing the bolus to leave the pharynx and enter the esophagus. In the case of a dysphagic patient, this muscle is impaired in its ability to maintain adequate width or duration of opening. This results in post-swallow pharyngeal residual, particularly in the pyriform sinuses. Additionally, prolonged increased pressure of the cricopharyngeal sphincter may contribute to the development of a Zenkers diverticulum immediately inferior to the muscle. The Mendelsohn Maneuver is a treatment strategy designed to facilitate cricopharyngeal sphincter opening. This strategy requires that the patient volitionally increase and maintain laryngeal elevation, thus stretching the cricopharyngeal sphincter. Since laryngeal elevation is the targeted movement, the muscles monitored are the same as those targeted for modified valsalva swallows, as mentioned above. This muscle group would specifically include the anterior belly of digastric muscle, the stylohyoid muscle and the mylohyoid muscle.
As with the modified valsalva swallow, the patient should initially receive a thorough explanation and demonstration of the treatment strategy. After electrode placement, the patient is instructed to identify the height of laryngeal elevation during the swallow and hold that position for several seconds before releasing muscular control and completing the swallowing cycle. The biofeedback line will shape boxes when the strategy is completed accurately (figure 7). The feedback line elevates off baseline with laryngeal elevation for initiation of the swallow, is maintained off the line while holding laryngeal elevation, then returns to the baseline with completion of the swallow. Treatment objectives include progressively increasing both the amplitude of the reading and the duration of elevation of the feedback line off baseline.
Relaxation of Pharyngeal Musculature
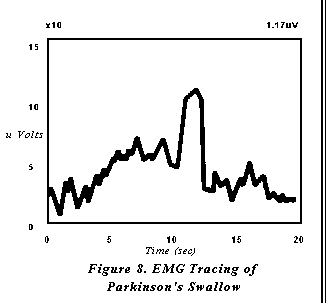
Several degenerative neuromuscular diseases result in dysphagic symptoms that require relaxation of pharyngeal musculature. In particular, Parkinsons Disease frequently results in a poorly coordinated, hyper-reactive response of pharyngeal contraction. A patient with this type of diagnosis may demonstrate adequate strength of contraction, but attempts to initiate the swallow results in a characteristic groping behavior. The patient may attempt laryngeal elevation for the swallow numerous times before actual onset and completion of the swallow. Thus, when a swallow is ultimately initiated, the effect is a weakened effort secondary to previously expended energy (figure 8). The result is an inefficient swallow with an increased risk for post swallow pharyngeal residual and malnutrition secondary to fatigue. In this case the muscles targeted are those responsible for laryngeal elevation (the suprahyoid muscle group). The target behavior is relaxation, rather than contraction, except during the occurrence of the swallow.
The objective of relaxing the pharyngeal musculature before and after the occurrence of a swallow is explained to the patient. After surface electrodes are applied, the patient is instructed to relax the muscles in the neck and throat until the biofeedback line is flat. The patient is then cued to swallow. The target behavior is a flat feedback line with a single peak for the swallow.
Conclusion
Several other authors have investigated the utilization of EMG in dysphagia diagnosis(6,7,8,12,13,15). These studies consist primarily of the application of subcutaneous needle electrode myography in the diagnosis of dysphagia and the scientific documentation of normal swallowing behavior. Further research in these areas is essential to the development of refined protocols for EMG applications. Subcutaneous electrode placement is generally not feasible or recommended for daily clinical practice; however, these studies can provide valuable information for the practicing clinician in refining surface electrode EMG biofeedback.
EMG biofeedback holds great potential as an adjunct to standard therapy for the rehabilitation of the dysphagic patient when under the direction of a speech language pathologist with expertise in this area. Biofeedback provides several critical elements that are unavailable with standard dysphagia therapy. Video monitoring allows the patient to view the swallow as it occurs, converting a previously automatic skill of which there is generally little awareness to a visually represented task that can be consciously monitored and altered. Target behavior and goal identification is measurable, providing the patient with invaluable insight into progress and motivation for continued treatment. And finally, quantitative data are produced to document the patients progress, facilitating reimbursement from third party payers. Swallowing therapy techniques are used to effect a change in the physiology of the oral and pharyngeal swallow. Biofeedback, if used appropriately, is a valuable patient aid in visualizing and documenting these changes.
REFERENCES