Oral-pharyngeal dysphagia is a common sequelae to a variety of acute and chronic illnesses, including cerebrovascular accident(16), traumatic brain injury(9), oral-pharyngeal carcinoma(2) and a myriad of degenerative neuromuscular diseases(5).
Swallowing impairment can result in significantly delayed recovery, malnutrition and dehydration(14), pulmonary complications leading to aspiration pneumonia and potentially death(3). Common deficits include weakness in the musculature of the lips, mouth, tongue, palate, pharynx and esophagus, incoordination of movements, surgical ablation of tissue and decreased sensation of the oral and pharyngeal cavities leading to a delay in the stimulation of the swallow(11).
In the past 5-10 years, there has been a significant movement toward rehabilitative treatment of dysphagia. Dysphagia intervention is utilized to both compensate for oral-pharyngeal swallowing impairment and to change the physiology of the swallow through muscle retraining, thus resulting in long term improvement in swallowing(11).
Many of the identified treatment strategies require that the patient translate a previously automatic physiological function into a volitionally controlled, altered motor response. For many patients, both those with and without associated cognitive impairment, grasping the concept of altering swallowing behavior is a challenge. There is little cognitive awareness as to how a swallow is executed. The swallowing therapist is consequently often confronted with confusion, frustration and an inability of the patient to participate in his or her own treatment.
EMG biofeedback presents auditory and visual signals to aid the patient in learning and practicing dysphagia intervention exercises(4). The EMG signal translates the previously automatic response into a concrete representation of oral-pharyngeal movement. Viewing the swallow as it occurs allows the patient to consciously monitor and alter swallowing behavior. The patient is able to clearly visualize the effects of specific compensatory and therapeutic strategies and target visible, realistically attainable goals. Additionally, in times of restrictions by third-party payers, EMG biofeedback provides quantitative data to document patient progress with treatment.
Treatment Protocol
Treatment of oral-pharyngeal swallowing impairment relies on accurate diagnosis. Thus any treatment protocol should be preceded by a thorough diagnostic evaluation by a qualified speech language pathologist. Specific exercises for the treatment of neurophysiological deficits have been described in the dysphagia literature(1,10,11). The scope of this protocol does not include an exhaustive description of dysphagic abnormalities and the associated treatment strategies of choice. It will encompass description of those treatment strategies that are appreciably enhanced by biofeedback monitoring.
Using MyoDac 2TM / MyoCompTM
The MyoComp System, as well as other computer assisted EMG Biofeedback Systems, allows for long-term storage of patient biographical, insurance and medical information on a separate diskette. This is accessed through the database mode on the main menu. In addition, a progress note section enables the therapist to store session information regarding the nature of treatment provided, the patients response to treatment, and other pertinent information. This information can be added to the diskette before or after a session through the monitoring mode on the main menu.
Setting on MyoDac 2TM
Setting on MyoCompTM System
- Options-as desired for auditory feedback and visual
contrast of EMG line on background.
Monitor
- For two channel tasks, use Channel 1 Top, Channel 2 Bottom.
- For one channel tasks, use Channel 1 Center.
- Time-as desired. A setting of 15 seconds provides
more responsive input to patients in the early stages
of treatment.
Single Channel Monitoring
For non-computerized monitoring or home training, the portable MyoTracTM single channel electromyograph can be used.
Oral Motor Facial Exercises
In cases of unilateral cerebrovascular accident or surgical resection and scarring from oral-pharyngeal carcinoma, facial weakness and asymmetry may inhibit adequate bolus control during feeding. Oral motor/facial exercises may be used to improve function in weakened muscles or to reduce constriction associated with scarring. Two muscles have been targeted for retraining with biofeedback. The orbicularis oris is a circular-appearing muscle that extends posteriorly from the buccinator muscle, with upper and lower muscle fibers inserting into the upper and lower lip. This muscle is functionally responsible in the deglutitive process for maintenance of the bolus within the oral cavity. The buccinator muscle is a flat band of muscle that provides the framework for the cheek. This muscle attaches at the pterygomandibular raphe with insertion into the orbicularis oris. The buccinator, combined secondarily with the masseter muscle, serves to tighten the cheeks during mastication and swallowing, inhibiting buccal pocketing. When the goal of treatment is to increase symmetry of contraction of the orbicularis oris and buccinator muscles, as in the case of unilateral cerebral infarcts, biofeedback can be used to assist the patient in matching the weakened musculature to the stronger intact side.
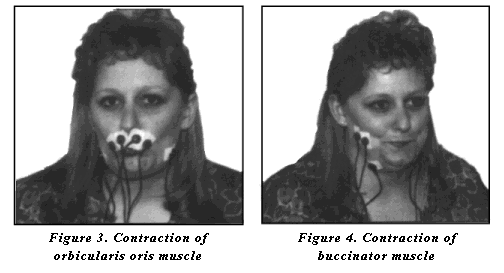
Electrode Placement: The EMG sensors are attached with surface single electrodes, connected to the MyoScan(TM) sensor with electrode extender leads. As functional-facial symmetry is the goal, two channels are used for the patient to target function of weakened hemiparetic side to parallel function of the stronger functioning side. The active electrodes are placed over the orbicularis oris or buccinator muscle with the ground electrode placed anterior to the muscle (figure 1 and 2). For work on lip closure, the function of both the upper and lower lip can be targeted; however, the upper lip is more accessible for secure electrode placement.
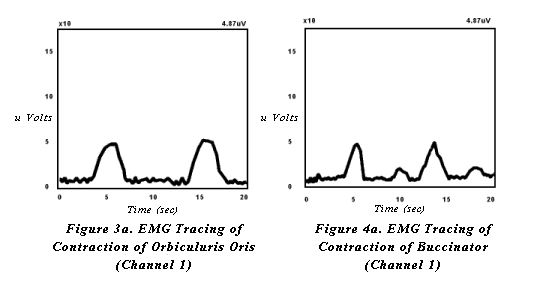
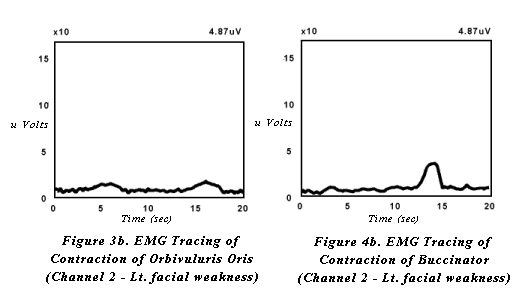
When targeting increased lip strength and closure, the patient is instructed to repetitively purse their lips then relax (figure 3). When targeting increased buccal tension, patients are instructed to tighten the cheeks against the teeth then relax (figure 4). Modeling of the task is usually required. With each contraction of orbicularis oris or the buccinator muscles and surrounding musculature, the patient will see a slope in the receiving, feedback line. The hemiparetic side will demonstrate decreased visual feedback (figures 3a, 3b and 4a, 4b). The goal for treatment is to shape the hemiparetic side to match the stronger, intact side of the face. Intermittent tactile stimulation may be applied by the therapist to increase sensitivity and response between volitional exercise.
Pharyngeal Phase Exercises