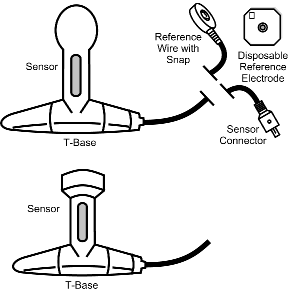
If "T" shaped sensors are used, the patient need not undress, and, if able, they should be allowed to insert the sensor themselves, taking care that the large end remains outside of the vagina or rectum. The "T" allows the patient to sit without any sense of discomfort and has the advantage of having the patient start training in a functional position making it easy to progress from sit to stand.
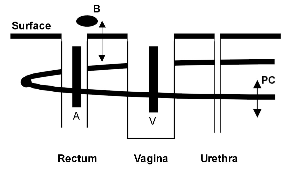
Figure 2: Longitudinal electrodes (A or V) of inserted sensors in close proximity to the pubococcygeus (PC) portion of the Levator Ani muscle.
Further, the seated position may enhance the patient's awareness of the pelvic floor if seated on a firm, surface. Rectal sensors are appropriate for male patients and some elderly women with small or atrophic vaginal openings. Some clinicians recommend a digital exam be performed by an appropriately trained and licensed clinician to rule out obstruction or impaction, prior to placement of a rectal sensor. The sensor, with a dab of KY JellyTM on the tip, should be gently inserted into the vaginal or anal canal, until all but the transversal end is inserted.
Before insertable EMG vaginal and anal sensors became widely available surface patch electrodes were placed near the anus to record muscle activity . However, as shown in Figure 2, the insertable sensor's electrodes lie much closer to both superficial ("A") and deeper ("B") segments of the pelvic floor muscles allowing for more sensitivity to the muscle activity.
Many clinicians find it valuable to assess and record initial resting baselines and voluntary contractions. A suggested assessment protocol follows:
The patient, fully clothed, is seated on a firm chair. This position allows for easy progression to a more functional standing position and further increases the patient's proprioception of the target muscles due to contact with the firm surface. The sensor is then connected to the EMG instrumentation.
Electrodes, monitoring accessory muscles, usually the abdominals, are attached by the clinician. These surface patch electrodes can be placed above the pubic symphysis and to the right of the umbilicus, 3-4 centimeters apart, to monitor muscle activity. After connecting to the EMG instrument, the assessment can begin. First, baseline information is gathered for the resting EMG levels of the pelvic floor muscles. The resting EMG levels should be acquired over a 1-3 minute interval.
Typically, a resting EMG reading under 2 microvolts rms is considered to be within normal limits, however, many patients will exhibit higher resting tones during the initial biofeedback visit and, occasionally, during the first few minutes of subsequent sessions. The patient is then asked to tighten the pelvic muscles and to hold the contraction for 10 seconds). The amplitude of the contraction will vary from patient to patient and is dependent on a variety of factors, including prior nerve or muscle damage to the pelvic floor as a result of childbirth or surgical trauma, genetic makeup of the individual, as well as placement of the electrodes and instrumental bandwidth. There is no "magic" number for signal amplitude during contraction and no evidence has been found to support any specific amplitude necessary to attain continence. Patients must be monitored on an individual basis. After the pelvic muscle contraction, a period of relaxation should follow, typically ten seconds. It is important that the pelvic muscles are isolated and that the accessory muscles of the legs, abdomen and buttocks are not contracted. The clinician may be able to observe this, but a second channel of EMG is necessary to rule out undesirable and often subtle activity from the accessory muscle groups. The clinician should instruct the patient to contract and relax the pelvic muscles four to six times, allowing for ten second rest periods between each contraction. These voluntary contractions should be observed for maximal amplitude, the average amplitude of the ten seconds, recruitment and fatigue. The resting levels should be observed for any evidence of muscle spasm, such as abnormally high resting tone, or even excessive activity at lower amplitudes. A response time, or measure of "latency", can be determined by recording the length of time it takes for the EMG signal to make the transition from rest to work and work to rest. These measures are typically 0.5 seconds for contraction and 1.0 seconds for relaxation.7 A series of five rapid, forceful contractions, sometimes called "quick flicks", are a good measure of the fast twitch fibers of the pelvic floor. The ability to perform 5 such rapid contractions in a ten second period is a goal in training patients to be able to use their muscles in a functional manner such as "squeezing" while coughing or sneezing. If using a computerized program, the display time on the polygraph screen can be set to show 2 minutes of activity, which will display all of the assessment information. The data can be saved, viewed on the screen or printed.
Biofeedback Technique for Pelvic Muscle Exercises
The biofeedback approach for treating urinary incontinence was pioneered by Arnold Kegel in the 1940's. His work was the basis for the pelvic muscle work being performed today. Currently, simple to use yet highly sophisticated EMG instruments monitor not only the pelvic muscles but the nearby accessory muscles, that patients frequently substitute in an effort to contract the seldom used, weak or damaged, muscles of the pelvic floor. The accuracy of sensors with longitudinal sensing electrodes, such as the Thought Technology sensors (Figure 1) have been shown to be virtually identical to the gold standard, inserted wire needle electrodes. Scottish researchers found that longitudinal electrodes correlated r=0.99, 0.99, and 0.91 respectively for rest, contract, and push-out strain, with traditional needle electrodes. They also found longitudinal electrodes to be considerably more sensitive to EMG signals than circular (i.e., electric stimulation) electrodes."
Just as in Dr. Kegel's day, patients continue to benefit from home training with biofeedback by using patient friendly EMG devices. There is some evidence that symptom reduction and elimination of urinary incontinence can be significantly enhanced through the use of such home training devices16.
There are several methods for training the pelvic floor musculature: