Through trial and error learning using a dual channel instrument, such as the MyoTrac 2TM or MyoTrac 3TM EMG system, EMG biofeedback permits one to isolate only the pelvic muscles. This is mandatory for further muscle training to continue. If a dual channel device is unavailable two single channel MyoTracTM or U-ControlTM units could be used. One of the instruments would monitor the abdominal muscles and the other, the pelvic muscles.
Muscle strengthening is done with maximal contractions, that are held for 5-10 seconds at a time, depending on the patient's ability, with 10-second rest periods in between. These work/rest cycles are repeated several times, until the contraction begins to show fatigue, or when the patient begins to compensate with accessory musculature. Endurance training is done with submaximal contractions held for increasingly longer periods of time.
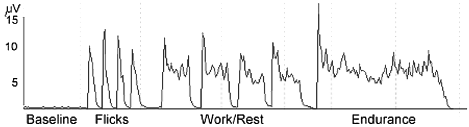
Speed of recruitment is practiced with several rapid forceful contractions (flicks) in a short time frame, for example, 5 successive contractions, performed within ten seconds. A progressive contraction can also be done, asking the patient to contract and relax gradually. The total time committed to actual biofeedback in a 45 minute appointment is approximately 15 minutes. The time spent on each type of training depends on the patient's problem and response. The remainder of the time is spent on patient education, review of voiding diary, and instruction in voiding schedules and dietary and fluid modification, as appropriate to each patient. A typical EMG signal for a similar protocol is displayed in Figure 3.
A review of the record keeping data, combined with a biofeedback session in the office or clinic, is usually suggested every 7-10 days with the healthcare professional. Initially, the patient is asked to practice at home, every day, with an exercise prescription based on her/his assessment in the initial session. For example, if the patient was only able to sustain a 4 second contraction during the first visit, it would be appropriate to prescribe home exercises in the following manner: contract for a count of 4, relax for a count of 10 for 5 repetitions. Repeat the preceding 5 times a day. The duration of the contractions should be increased until the patient is able to sustain for a full 10 seconds. As the patient progresses, or, initially, if appropriate, two or three EMG feedback sessions can be prescribed using a home unit. It is imperative that the patient be able to isolate the pelvic muscles consistently before using a single channel device for home practice. Additional non-instrumented muscle contraction exercises are also given, based on the patient's performace within the clinical setting. These can be tailored to suit the patient's individual lifestyle, taking into consideration that busy schedules may hamper compliance. The literature shows that 30 to 80 contractions, daily, are sufficient to improve pelvic muscle function thus reducing incontinent episodes. There are a variety of other suggestions available in the literature. A workable schedule, for many patients, has been 5 or more sets of 5 repetitions throughout the day. A commitment of 11/2 -2 minutes for exercise, several times a day, is agreeable to most patients without disturbing their routine to the point of non-compliance. During subsequent weeks, these exercises should be practiced with increasing duration and effort, with changes in position during exercise.
If working with a child or an infirmed elderly patient, the assistance of a parent or attendant may be helpful. Clear instructions as to the frequency of practice and maintenance of any instrument, sensor or equipment should be given.
A continuation of the daily records should be kept throughout the training period. These should include episodes of incontinence, degree of activity during episode as well as occasions of toileting without accident. Once the biofeedback training sessions are complete and symptoms have resolved, it is imperative that the patient continue muscle contraction exercises to maintain the effective muscle function and symptom resolution.
Several choices of monitoring instruments are available. Single or dual portable EMG systems, which provide audio and/or visual feedback, are ideal for home training. A more sophisticated computerized data acquisition system is recommended for clinical assessment.
Conclusion
Incontinence is an extremely prevalent disorder. Biofeedback has had a great impact upon incontinence, due to its ease of use, low cost and very high success rate. Most patients can use EMG biofeedback successfully at home. Although treatment time varies, in most people, continence can generally be restored in 4-8 weeks for both fecal and urinary incontinence by using the techniques described in this protocol, which combine clinical assessment and training with EMG biofeedback.
References
-
N.R. Binnie, B.M. Kawimbe, M. Papachrysostomou, N. Clare, and A.N. Smith, "The importance of the orientation of the electrode plates in recording the external anal sphincter EMG by non-invasive anal plug electrodes", Int. J. Colorect. Dis. (1991) 6:5-8.
-
Bo, Kari, et al: Pelvic Floor Muscle Exercise for Treatment of Female Stress Urinary Incontinence, Neurology and Urodynamics 9:471-477, 1990.
-
Burns, Patricia, et al. Treatment of stress incontinence with pelvic floor exercises and biofeedback. J.A.G.S. 38: 341-344, 1990.