Erik Peper, Ph.D.
San Francisco State University,
San Francisco, CA
Vietta S. Wilson, Ph.D.
York University, Toronto, ON
Will Taylor, M.D.
Blue Hill, ME
Alex Pierce,
Stens Corporation, Oakland, CA
Kathy Bender,
SHARE, Oakland, CA
Vicci Tibbetts,
San Francisco State University,
San Francisco, CA
Introduction
Improper work habits, poor workstation ergonomics, and environment can lead to physiological dysregulation such as muscle soreness, fatigue, and injury (Grandjean, 1987). Some workers develop chronic neck and upper limb pain also known as repetitive strain injury. (RSI), cumulative trauma disorder (CTD) or overuse syndrome, from long hours of repetitive tasks at personal computer workstations. Workers with RSI suffer loss of productivity and income with increasing medical costs. RSI accounted for forty percent of workers compensation cases in 1990. Discomfort and injury can shape the way PC users feel about their job and computers. Forty million Americans use computers, and 15-20 percent are at risk for RSI symptoms (CDC, 1984). RSI threatens to inflict individuals with illness and overwhelm corporations with increasing medical costs and lost productivity.
At present, workstation ergonomic analysis, proper positioning of furniture and equipment, different mice and keyboards, and periodic rest may help reduce physiological dysregulation (the incidence of muscle fatigue or injury). This mechanical approach, however, lacks two crucial elements:
- Kinesthetic awareness of psychophysiology by computer users.
- Development of skills to inhibit inappropriate and excessive bracing during task performance.
The computer user must learn to reduce tension and relax muscles when they are not used for the task. Preventing RSI involves a combination of proper ergonomics, work pattern variation (work/rest cycle), and self-regulation through biofeedback to reduce dysponetic activity (inappropriate and misdirected, as well as unconscious muscle bracing). Without kinesthetic awareness and without the skills to reduce tension, ergonomic adjustments with intermittent rest periods are NOT sufficient to reduce risk for injury.
Computer users can learn preventative skills to sense muscle tension and incorporate relaxation and regeneration of muscles during data entry and mouse use. Biofeedback instruments can be used to monitor specific muscle sites and to warn the user of excessive strain or overuse habits that can lead to chronic pain or injury. This mastery process reduces the risk of RSI.
RISK FACTOR ANALYSIS
The development of RSI involves ergonomic and psychophysiological contributing factors which include:
- Inappropriate ergonomic workstation setup
- VDT (monitor) induced near-vision stress
- Asymmetrical task performance
- Restricted body movements
- Absence of brief (1-2 seconds) regenerative breaks during work activity (micro-breaks)
- Dysponesis during task performance (co-contraction, lack of inhibition of antagonist during movement)
- Lack of somatic awareness of tension and relaxation
- Physiological tension during self-perceived relaxation
- Excessive focus on tasks and or flawless work record
- Work dissatisfaction
- Frequent previous illnesses
- Excessive physiological reactivity
- Thoracic breathing and/or breath holding during data entry
- Presence of tender trigger points
The following RSI protocol includes ergonomic and work style evaluation, psychophysiological profile, risk factor analysis, biofeedback training and education.
ERGONOMIC AND WORK STYLE EVALUATION
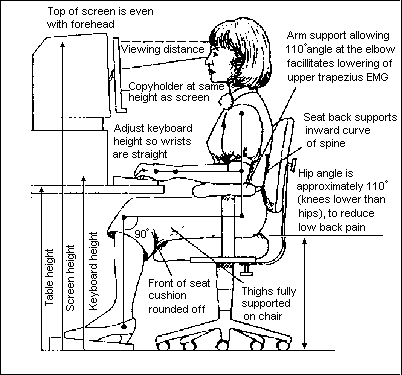
Ergonomic evaluation needs to be done at the work site under normal working conditions. (Compare the computer user position to the recommended guidelines, see Fig. 1.) The attached assessment form, SFSU WORKSTATION AND ERGONOMIC ASSESSMENT (Peper and Tibbetts, 1994) can be used as a guideline to cover most of the ergonomic risks (see also Jones, 1991; State of California, 1993). At the same time, movement analysis of task performance needs to be included because repeated asymmetrical movements increase risks (Donaldson, 1994). A table of typical computer user complaints, corresponding ergonomic factors, and areas for surface electromyography (sEMG) are listed in Table 1 (Wilson, 1994).
Figure 1.
Workstation arrangement to reduce risk of discomfort.
(Illustration, courtesy of Great Performance, Inc.
(800)433-3803).
After evaluation, ergonomic risks are identified and solutions proposed. Many solutions can be economical, such as lowering the monitor by placing the computer sideways on the floor, lowering the keyboard by attaching a keyboard drawer, raising the feet by using telephone books, and removing boxes or waste basket from under the desk so that the legs are free to move. Sometimes, the solution requires a reorganization of the office, such as moving office furniture, to reduce excessive reaching, or to allow distant vision.
In cases of asymmetrical job patterns, the person is guided to do the job alternately using opposite sides of the body, as well as changing the position of furniture (phones, files) to balance movement patterns. For example, during the morning, place the phone on the left side and lift the receiver with the left hand, while during the afternoon, place the phone on the right side and use the right hand.
An additional factor commonly overlooked is appropriate vision correction, especially for people who wear bifocals. Prescribed reading glasses (often used at the computer) force the user to tilt the head back or hunch forward since the focal distance is not set at the distance of their workstation monitor (Grandjean 1987). Some users may need to have special computer monitor reading glasses.
Equally important, computer users need to be aware of the work/rest cycle. This means both very short breaks and movements during task performance and larger body movements during frequent longer breaks.
PSYCHOPHYSIOLOGICAL PROFILE
After ergonomic assessment and adjustments, a physiological assessment should be done. If possible, it should include an actual work site assessment, which can easily be done with a laptop computer and a portable two channel EMG device like Thought Technology's MyoTrac2(TM) or ProComp+(TM) systems. The comprehensive profile consists of different phases which can also be selectively used depending upon the computer user's needs.
The psychophysiological profile consists of physiological monitoring during: a) task performance, b) simulated emotional stress, c) extended data entry, and d) movement symmetry. The purpose is to assess dysponetic activity (misdirected and inappropriate bracing patterns), the length of short breaks, the effect of emotional stress upon physiological reactivity, physiological recovery, asymmetrical muscle co-contractions, and somatic awareness.
The profile assesses the individual at the computer, either at the job site or at a simulation of the workplace setting. The data entry task needs to include the actual data entry pattern of the user (e.g. keyboard, mouse, and/or trackball). The initial assessment does not include feedback, although all the data is recorded for later analysis.
IMPORTANT: The protocol should be adapted to assess real task performance such as job related data entry, reaching for the phone with the right and left hand, etc.
After the protocol has been completed, the data can then be reviewed with the client to show the individual's physiological responses. This information is then used to determine self-regulation strategies to improve health. This feedback is usually done directly after the assessment so that the information can be used to begin retraining.
SENSOR REQUIREMENTS AND PLACEMENT
The minimum requirement for the assessment is two channels of surface electromyography (sEMG). A two channel sEMG assessment will require moving sensor leads to different muscle sites during different phases of the assessment. A more comprehensive assessment would include a minimum of 4 channels of sEMG, respiration, skin temperature (Temp) and skin conductance response (SCR).
Two channel sEMG sensor placement:
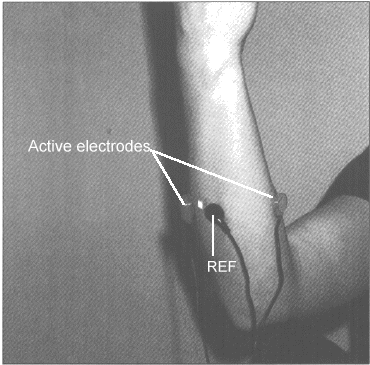
A) Forearm sEMG: Place the
active electrodes midpoint on the extensor and flexor muscles
(see Fig. 2) to monitor forearm tension. The purpose for
monitoring the forearm is that most subjects do not relax the
fingers or wrist muscles as long as the fingers are on the
keyboard or holding the mouse.
Figure 2. Forearm
sEMG sensor placement
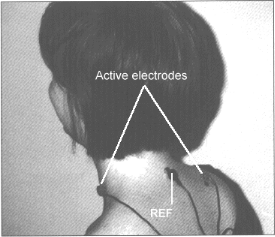
B) Neck and shoulders sEMG: Place one active electrode over the left scalene and the other, midpoint on the right trapezius (see Fig. 3). The purpose of monitoring the neck and shoulders is that most subjects raise their shoulders and tend toward thoracic breathing patterns during task performance. The left scalene to right trapezius placement will also monitor bracing by the scalene and sternocleidomastoid muscles.
Figure 3. Neck and
shoulder sEMG placement
Four channel sEMG sensor placement:
Sensors are placed to allow bilateral analysis during the symmetry assessment. The most common bilateral electrode placements (right and left) include the following muscles: upper trapezius, lower trapezius, sternocleidomastoid, rhomboid, and pectoralis. The purpose for monitoring upper and lower trapezius is to enhance scapular stabilization since the lower trapezius will inhibit the upper trapezius activity. (For exact electrode locations see: Soderberg, 1992: This manual is free and available from NIOSH, see recommended sources for more information; and Basmajian & Blumenstein, 1980).
Comprehensive monitoring
includes thoracic and abdominal respiratory patterns and
breathing rate, peripheral temperature, skin conductance, and
heart rate. Monitoring should also include the following sEMG
placements, bilateral cervical paraspinals, masseters, temporalis, deltoid, upper and lower
trapezius, pectoralis, infraspinatis, wrist extensors and flexors, and possibly,
tibialis and gastrocnemius.
ASSESSMENT PROTOCOL
- Describe the protocol sequence.
- Have the person sit comfortably at the computer station. (Do the ergonomic assessment and modifications as needed)
- Attach physiological monitoring device and verify signals.
- After each step of the assessment, have the person rate their subjective stress/tension.
PHASE 1:
Effect of Position and Task on Physiology
PURPOSE:
To assess subjective muscle tension awareness, posture and
task performance upon the physiology.
PROCEDURE:
- Sit comfortably with hands resting on lap (30 seconds baseline).
- Place fingers comfortably (their normal mode) on the keyboard at home row (30 seconds).
- Type a standard text (a sample letter or materials that simulate a normal job task) (60 seconds).
- Place fingers comfortably on the keyboard without pressing keys (30 seconds).
- Place hands back on lap comfortably in a relaxed position (30 seconds baseline).
RISK PATTERNS:
The following are common physiological patterns which may be
identified and may increase risk (Fig. 4).
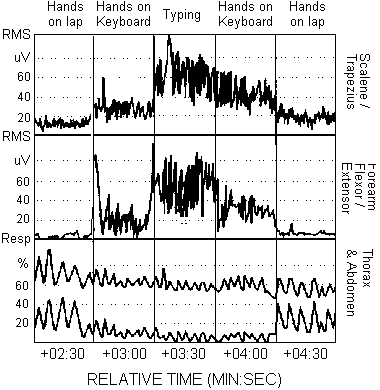
Figure 4. Common
Dysfunctional Physiological Patterns include: Increased scalene/trapezius sEMG activity when the hands are on the
keyboard and during typing. Increased forearm flexor/extensor
sEMG activity when the hands are on the keyboard. Absence of
micro-breaks (low sEMG epochs) when typing. Increased
respiration rate when the hands are on the keyboard and when
typing. Decreased abdominal expansion while breathing when
hands are on the keyboard and when typing.
- Absence of regenerative micro-breaks (1-2 seconds epochs of low sEMG activity every 10-20 seconds) from activated muscles.
- Increased scalene/trapezius sEMG activity when the person's fingers are on the keyboard. (Covert dysponesis: the person is unaware the shoulders are raised when preparing to type.)
- Increased forearm sEMG activity as long as the fingers are on the keyboard. (The sEMG increased even when the person thought the arms and hands were relaxed at the keyboard.)
- Increased respiration rate and thoracic breathing when the person types (increased nervous arousal) and decreased respiratory sinus arrhythmia.
- Increased sEMG activity, increased respiration rate and thoracic breathing after hands are placed back on lap (lack of or slow recovery).
- Low correlation between subjective sense of stress/tension rating and sEMG activity.
PHASE 2:
Effect of Emotion on Physiology
PURPOSE:
To assess the impact of negative emotions upon physiology.
PROCEDURE:
- Sit comfortably in front of the computer, hands on lap.
- Think, feel, imagine, visualize an angry, resentful, and frustrating job-related or personal experience and indicate when these angry/resentful feelings/thoughts are present.
- Continue to experience the negative feelings/thoughts with hands on lap (30 seconds).
- Continue to experience the negative feelings/thoughts, and type a standard text (60 seconds).
- Let go of the negative feelings/thoughts and rest/relax with hands on lap (60 sec. baseline).
RISK PATTERNS:
The following are common risk patterns, in addition to those
described in PHASE 1, which need to be retrained (Fig. 5).
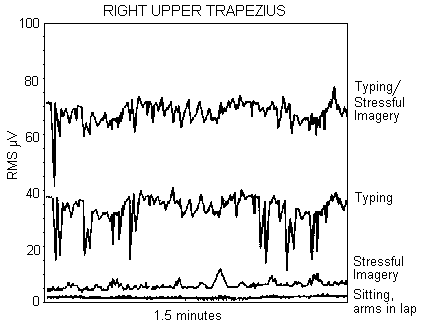
Figure 5. The effect of stressful imagery on right upper
trapezius muscle activity. Note that there are NO
micro-breaks during the typing with stressful imagery, while
there are micro-breaks (epochs of low EMG) during the normal
typing task. In addition, the EMG activity is significantly
increased during stressful imagery in both the sitting, arms
in lap, and the typing conditions.
- Increased sEMG activity and arousal during typing as compared to PHASE 1 baseline and typing tasks.
- Slow recovery back to baseline measures following the instructions of letting go of the negative imagery while resting hands on lap.
PHASE 3:
Effect of Continued Task Performance on Physiology
PURPOSE:
To assess the impact of long duration work pattern upon
physiology.
PROCEDURE:
- Sit comfortably with hands resting (relaxed) on lap (1 minute baseline).
- Type a standard text (a sample letter or materials that simulate a normal job task) (10-50 minutes).
- Sit comfortably with hands resting (relaxed) on lap (1-5 minute baseline).
RISK PATTERNS:
The following are common risk patterns, in addition to those
described in PHASE 1 and 2, which need to be retrained.
- Sustained upper trapezius sEMG activity lasting longer than 30 seconds without the presence of regenerative micro-breaks (1-2 seconds of very low sEMG activity) (3).
- Increased scalene/trapezius sEMG during data entry without micro-breaks.
- Increased forearm sEMG while the fingers are on the keyboard.
- Increased respiration rate and thoracic breathing during data entry.
- Slow recovery back to baseline measures following typing task.
- Absence of gross body movements.
PHASE 4:
Symmetrical Movement Analysis for Muscle Co-Contraction and
Recovery Analysis
PURPOSE:
To assess sEMG
imbalance during movement patterns (Taylor, 1993; Wilson,
1994; and Skubick, Clasby, Donaldson, & Marshall, 1993;
Donaldson, 1994).
PROCEDURE For SCM sEMG
assessment:
SENSOR PLACEMENTS:
Use two or four EMG channels, place sEMG active sensors on
the right and left sternocleidomastoid (SCM) (optional: right
and left upper trapezius)(Fig. 3).
- Sit comfortably in front of the computer with the hands on lap, while looking straight ahead (5 seconds).
- Rotate head to the right, as if looking over the right shoulder, while keeping the torso facing forward (5 seconds).
- Rotate head to face forward (5 seconds).
- Rotate head to the left, as if looking over the left shoulder, while keeping the torso facing forward (5 seconds).
- Rotate head to face forward (5 seconds).
- Repeat rotation sequence 5 times.
ALTERNATIVE MOVEMENT
PATTERN:
Have person perform real job tasks such as reaching for the
phone, manuals, or turning pages with one hand and then with
the other hand. Repeat movement 5 times.
PROCEDURE For upper
trapezius assessment:
SENSOR PLACEMENTS:
Use two or four EMG channels, place sEMG sensors on right and
left upper trapezius (optional: right and left SCM).
- Sit comfortably in front of the computer with the arms and hands hanging along the sides of the body with the palms facing toward each other (5 seconds).
- While keeping the elbow straight, lift both arms up until they are horizontal (90 degrees to the body) and hold for 6 seconds. Then return the arm to hang along side the body. (In this movement, the palms initially point towards the floor.)
- Repeat movement sequence 5 times.
ALTERNATIVE MOVEMENT
PATTERN:
Have person perform movements which mimic common job
movements.
OPTIONAL:
Repeat one cycle of the above movement patterns while
changing the time duration 30-60 seconds at the full
extension. (Do not continue if pain occurs.) Allow at least
120 seconds for recovery between right and left movements.
RISK PATTERNS:
The following are common risk patterns, in addition to those
described in PHASE 1, 2, and 3, which need to be retrained.
- Asymmetry in sEMG activity during movement. For example, right SCM sEMG significantly higher when head turns left than left SCM when head turns right or vise versa; similarly, asymmetry in sEMG trapezius activity when arms are moved upward.
- Significant co-contraction of antagonist during rotational movement. For example, left SCM sEMG is activated while head turns to the left.
- Breath holding or very shallow breathing during movements.
- Lack of awareness of breath holding.
- Lack of awareness of co-contraction and asymmetrical muscle use patterns.
- Slow sEMG recovery to baseline after five repetitions or after longer holding.
Data Review
Review the recorded data from the assessment protocol. Identify physiological response patterns and work habits which may increase the risk of RSI. The most commonly observed risk patterns are the absence of muscle tension awareness (awareness of muscle tension does not correlate with sEMG activity), inability to relax muscles, dysponesis (bracing of the trapezius during data entry), increased arousal during data entry, absence of regenerative micro-breaks during typing tasks (see Figs. 4 and 5), asymmetry and co-contractions during movement, and absence of gross body movement patterns.
Training and Education
The training protocol consists of reducing the observed risk patterns and generalizing these new skills into the persons work behavior. If significant dysponesis is observed, a more detailed sEMG analysis of specific muscles is required. The more specific the feedback, the more successful will be the skill acquisition.
The general training themes consist of increasing awareness of dysponetic activity, inhibiting co-contraction by tightening the correct agonist and inhibiting the antagonist, encouraging regenerative micro-epochs of very low sEMG activity of an activated muscle, reducing arousal (startle) during data entry through methods such as continued breathing, developing movement patterns using both sides of the body equally, and teaching that health consists of the alternation between activity and regeneration (movement and relaxation). The training goals are enhanced when monitored with portable EMG trainers (MyoTrac and MyoTrac2) or computer based systems (ProComp, FlexComp or MyoTrac2). The general psychophysiological concepts to achieve training goals are:
- Encourage lowering of arousal during task performance and breaks.
- Teach diaphragmatic breathing to reduce hyperventilation (Peper, 1990).
- Teach momentary regenerative breaks during continued task performance. Sustained muscle activity of greater than 30 seconds needs to have regenerative epochs (1-2 seconds) of low EMG activity. The micro-breaks are much more important than the muscle tension during the task (Taylor, 1993).
- Develop muscle strength, flexibility and bilateral symmetry appropriate for task performance through movement exercise and workstation rearrangement (Wilson, 1994).
CAUTION: Any numbness, tingling, prickling sensation or loss of sensation or dropping of objects should be evaluated by a physician. These symptoms are most prevalent in the early morning, evening or wakes the person from sleep.
TRAINING GOALS:
A. OPTIMIZE ERGONOMIC CORRECT POSITION
- Implement the ergonomic improvements derived from the ERGONOMIC WORK STYLE EVALUATION.
- Optimize body position at the work station with sEMG monitoring. For example, place sensors on deltoid or trapezius to identify the neutral arm position while hands are on keyboard (Fig. 6) (Peper and Shumay, 1994).
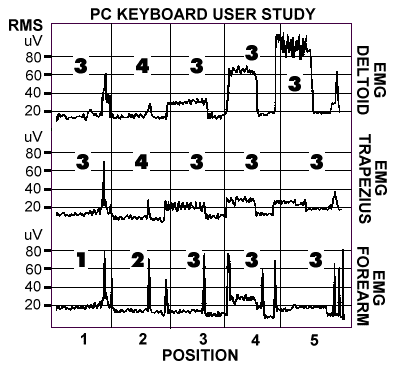
Figure 6. The use of sEMG from right trapezius, deltoid,
and forearm to optimize keyboard location. Position 1 is
resting with hands on lap, position 2 is most ergonomically
correct with hands at keyboard, while position 3, 4, and 5
are ergonimacally incorrect. NOTE that there is NO
correlation between sEMG activity and subjective awareness of
tension as indicated by the numerical scores (1 - most
relaxed to 5 - most tense) for each position and shoulder and
forearm body locations.
B. EMG GOALS
- Inhibit scalene/trapezius sEMG activity while fingers are on the keyboard during rest and data entry. This means the person learns to sense bracing in the shoulders and lets the shoulders stay relaxed during data entry.
- Inhibit finger/wrist flexor/extensor sEMG activity when fingers are resting on keyboard.
- Inhibit shoulder girdle and arm bracing (excessive sEMG activity) while using a mouse.
- Inhibit sEMG co-contraction of muscles such as SCM.
- Teach scapular stabilization utilizing lower trapezius and serratus anterior sEMG feedback to inhibit upper trapezius activity (Bender, 1993).
- Monitor sEMG and inhibit dysponetic activity from relevant muscle groups while performing job related keyboard entry tasks.
C. RELAXATION/STRENGTHENING PRACTICES
- Head rotations: SLOWLY look over right shoulder. Hold 20 seconds, back to center. Repeat on the other side. (Minimize shoulder movement as much as possible.)
- Side headbends: Put right ear to right shoulder. Hold 20 seconds, back to center. Repeat on other side (minimize shoulder movement as much as possible).
- Turkey pull: GENTLY pull your neck backwards as if someone had a string attached to the back of your neck and was pulling it backward. Keep the jaw parallel to the ground and shoulders relaxed. Do 2-30 times daily.
- Shrug shoulders backward and forward in a circular motion, go slowly. Several circles should be executed-- each of a different diameter.
- Place arms at sides as if you were standing at attention. Keeping arms as straight as possible, raise them up over your head until the backs of your hands meet above your head. Ensure that palms face down as arms extend. The action should look like a slow motion jumping jack (or a very lethargic duck trying to fly). Do not arch lower back.
- Do Dynamic Relaxation of the neck, shoulders, arms, wrists, hands, and fingers (Peper and Holt, 1993). Teach internal mastery of high and low muscle tension and the ability to relax the muscle at will.
- Take brief 1 to 2 seconds regenerative breaks every 30 seconds during keyboard data entry and mouse use. For example, drop hands to the desk top or lap, the sEMG of the neck and shoulders should instantly return to low baseline levels.
D. EMOTIONAL CONTROL
- Enhance awareness of how negative emotions contribute to dysfunctional patterns.
- Develop communication and problem solving skills to resolve work and/or family conflicts.
- Teach thought stopping and/or task focusing exercises.
E. IMPLEMENTATION
- Generalize the above learned skills while performing relevant keyboard entry tasks at the actual job site.
- Breathe diaphragmatically and decrease breathing rate during relevant task performance.
Suggestions and Implications
Every person who uses or begins to use a computer should be instructed in somatic awareness, proper ergonomics, and rest/activity cycles. For many people, a signal from a small portable sEMG feedback device can help facilitate awareness of dysponesis during data entry and mouse use. Both the MyoTrac and MyoTrac2 devices (from Thought Technology Ltd.), offer the option for delayed tone feedback. This delayed feedback ignores the normal stretching, yawning, and other brief movements, whereas sustained sEMG activity triggers a warning feedback tone. In addition, external reminders to trigger brief regenerative breaks, as well as, encouraging episodic body movements may reduce the risk of RSI (e.g., timed alarms or automatic data entry interrupts). Finally, this protocol can be used to teach computer users preventative skills to avoid RSI and mobilize health. Table 1:
TYPICAL COMPUTER USER COMPLAINTS, CORRESPONDING ERGONOMIC FACTORS AND SUGGESTED MUSCLE GROUPS FOR SENSOR PLACEMENT
| HEAD | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Eye
strain: Pain or fatigue |
VDT
distance and tilt Lighting Optical prescription |
Frontalis/posterior
neck Temporalis Suboccipital Frontal |
| Headache | Telephone
usage Rest breaks from VDT Sitting posture Squinting Clenching teeth Fumes of toner Fluorescent lights |
Frontal/posterior
neck Temporalis Masseter Suboccipital Cervical paraspinal Trapezius Sternocleidomastoid |
| NECK AND SHOULDERS | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Headache back of head or neck |
Document
position (flat) Distance from VDT (too far) Head off-center Arms not supported Bifocals |
Frontal/posterior
neck Trapezius Masseter Sternocleidomastoid |
| Pain in shoulders | Head
tilt (display too high or too low Bifocal glasses Hunched shoulders (keyboard height too high) Drooped shoulders (too far away from keyboard. no muscle tone) Mouse distance One-sided movements |
Trapezius Deltoid Pectoralis Infraspinatus Scalenes |
| ARMS, WRISTS AND FINGERS | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Elbow pain | Repetitive
motion/no rest Keyboard design Mouse distance |
Triceps Brachioradialis Forearm extensors Scalenes |
| Wrist pain | Repetitive motion/no rest | Upper
shoulder Sternocleidomastoid Brachioradialis Forearm extensors Scalenes |
| Finger pain | Repetitive motion/no rest | Digital
Extensors Forearm extensors Scalenes |
| BACK | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Lower back or hip pain | Chair
(lumbar support) Posture Leg Position Feet on floor (sloped rest) High/low hip or shoulders Hip beneath knee |
Upper
back Lumbar region |
| LEGS, ANKLES AND FEET | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Elbow pain | Repetitive
motion/no rest Keyboard design Mouse distance |
Triceps Brachioradialis Forearm extensors Scalenes |
| Wrist pain | Repetitive motion/no rest | Upper
shoulder Sternocleidomastoid Brachioradialis Forearm extensors Scalenes |
| Finger pain | Repetitive motion/no rest | Digital
Extensors Forearm extensors Scalenes |
| BACK | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Lower back or hip pain | Chair
(lumbar support) Posture Leg Position Feet on floor (sloped rest) High/low hip or shoulders Hip beneath knee |
Upper
back Lumbar region |
| LEGS, ANKLES AND FEET | ||
| Typical complaints | Possible ergonomic factors | Areas of sEMG placement |
| Pain down the leg | Compression
from chair (inadequate padding on bottom, sharp front edge) Leg position (crossed legs or sharp leg bend One side movement |
Hamstrings Glutei Piriformis |
| Swollen ankles | Lack of movement | |
| Pain in foot or toes | Feet
not on floor/sloped rest Poor circulation Leg position Lack of movement |
|
SFSU
WORKSTATION AND ERGONOMIC ASSESSMENT
(Peper & Tibbets, 1994)
Instructions: Observe and circle possible risk factors.
Name: ____________________ Date: _____________ Rater: ____________________
Monitor 80 degrees from eye
position High ___ Low ___
Distance 3
feet
Near ___ Far ___ ?
___
Position
Left ___ Right
___ ? ___
Glare and reflexion
Yes ___ ? ___
Bright
lights
Yes
___ ? ___
Needs larger
screen
Yes ___ ? ___
High.clear screen resolution No
___ ? ___
Ability to look at a far object No
___ ? ___
Glasses-bifocals
Yes ___ ? ___
Contacts
Yes ___
? ___
Uses reading/computer glasses Yes
___ ? ___
Position of reading material Near ___
Far ___
High
___ Low ___
Comments:________________________________________________________________
Chair Feet reach
floor
No
___ ? ___
Thighs
compressed
Yes ___ ? ___
Seat angles
back
Yes ___ ? ___
Back
support
No ___
If present, is it
used?
No ___
? ___
High ___ Low ___
Arm
rests
Yes ___
Lifts
shoulders
Yes ___
? ___
Comments:________________________________________________________________
Legs Enough room for
feet
No ___ ? ___
Space for leg
movement
No ___ ? ___
Angle of knees at 110o
No ___ ? ___
Foot
support
No
___ ? ___
If present, is it
used
Yes ___ No
___
Sometimes ___
Comments:________________________________________________________________
Keyboard
Adjustable
No ___ ? ___
High ___ Low ___
Stable
No ___ ? ___
Wrist
pad
No ___ ? ___
Hard ___ ? ___
Comments: _____________________________________________________________
Arms Angle of upper arm
(vertical) Forward ___ Backward ___
Angle of forearm at elbow (110o) Smaller ___ Greater ___
Elbows
out
Yes ___ ? ___
Angle of
hand
Flexed ___ Extended ___
Finger
nails
Long
___ ? ___
Types with finger
nails
Yes ___ ? ___
Tension visible (tendons, fingers) Yes
___ ? ___
Comments: _____________________________________________________________
Mouse/
Present
Yes ___ ? ___
trackball Frequency of
use
Often ___ Sometimes___
Location
Distant ___ ? ___
Reaches out to
side Yes
___ ? ___
Reaches out
forward Yes
___ ? ___
Comments: _____________________________________________________________
Phone Frequency of
use
Often ___ Sometimes___
Duration of
use
___ Minutes
Twists for
use
Yes ___ ? ___
Location
Distant ___
Shoulder
rest
No ___ ? ___
Headset
No ___
? ___
Writing.data entry during calls Yes
___ ? ___
Comments: ___________________________________________________________
Space Enough room on
desk
No ___ ? ___
Office space
personalized No
___ ? ___
Back to
door
Yes ___ ? ___
Comments: _____________________________________________________________
Work habits Takes breaks every 15-30
min. No
___ ? ___
Does multiple body
movements/task No ___ ? ___
Assymetrical movements during task
Yes ___ ? ___
Reaching during
work
Yes ___
? ___
Mini-breaks during keyboard
entry No
___ ? ___
Percent time at
computer
<25% 50% 75%> ? ___
Previous workstation assessment
and/or suggestions
implemented? No
___ ? ___
Comments: ____________________________________________________________
Personal
Clothing
tight ___ ? ___
Belt (waist
constricted)
Yes ___ ? ___
Stationary (abscence of movement) Yes
___ ? ___
Thoracic breath
pattern
Yes ___ ? ___
Shifts to thoracic breath
pattern while
working
Yes ___
? ___
Skewed posture while
sitting
Yes ___ ? ___
Startle
posture
Yes
___ ? ___
Conscientious/driven
Yes ___
? ___
Hands
Cold ___ Moist ___ ? ___
Smoking
Yes ___ ? ___
Comments: ___________________________________________________________
Workstation adjustment suggested: ________________________________________
__________________________________________________________________________
__________________________________________________________________________
__________________________________________________________________________
Changes in work habits suggested: _______________________________________
__________________________________________________________________________
__________________________________________________________________________
__________________________________________________________________________
Psychophysiological profile appointment date: _________________________________
RECOMMENDED SOURCES
Basmajian, J.V. & Blumenstein, R. (1980). Electrode Placement for EMG Biofeedback. Baltimore: Williams & Wilkins.
Cram, J. (Ed). (1989). Clinical EMG for Surface Recording. Nevada City, CA: Clinical Resources.
Grandjean, E. (1987). Ergonimics in Computerized Offices. New York: Taylor and Francis.Peper, E. (1990) Breathing for Health. Montreal: Thought Technology Ltd.Soderberg, G.L. (Ed). (1992).
Selected Topics in Surface Electromyography for use in the Occupational Setting: Expert Perspectives. U.S. National Institute for Occupational Safety and Health, Publication No. 91-100. Available from NIOSH Publications, Mail Stop C-13, 4676 Columbia Parkway, Cincinnati, Ohio 45226-1992. State of California, Department of Personnel Administration. (1993). Video Display Terminal (VDT) Users Handbook. Sacramento, CA.
Travell, J.G. & Simons, D.G. (1983). Myofascial Pain and Dysfunction: The Trigger Point Manual. Baltimore: Williams & Wilkins.
Whatmore, G. and Kohli, D. (1974). The Physiopathology and Treatment of Functional Disorders. New York: Grune and Stratton, 1974.
Footnotes:
- A number of the concepts in this protocol have been derived and expanded from the contributions made by Donaldson & Skubick, 1993; Ettare & Nadler, 1993; and Middaugh et al, 1993. We thank Cathy Holt, Dianne Shumay, and Scott Davis for their helpful contributions.
- Reprint requests contact: Erik Peper, Ph.D., Institute for Holistic Healing Studies, San Francisco State University, 1600 Holloway Ave, San Francisco, CA 94132. FAX: 415-338-0573; EMAIL: epeper@sfsu.edu.
- Ergostats by Will Taylor, M.D., software to analyze sEMG recordings for regenerative micro breaks is available from biofeedback distributors.
Copyright, 1997 The Biofeedback Foundation of Europe